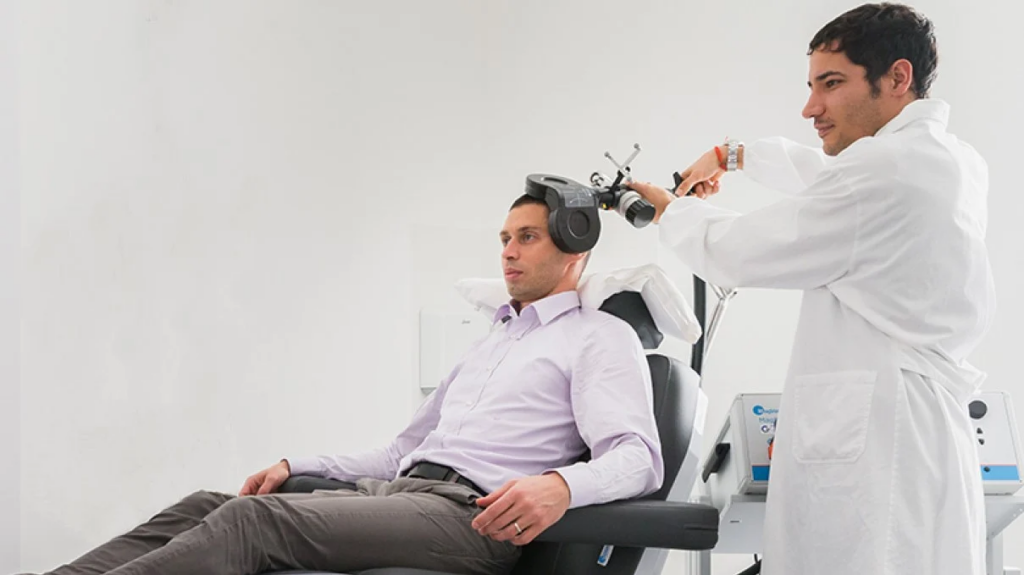
Transcranial Magnetic Stimulation (TMS) for depression is a non-invasive, evidence-informed treatment used to support adults experiencing depressive symptoms that have not responded adequately to traditional approaches. Unlike medication-based treatments, TMS uses targeted magnetic pulses to stimulate specific areas of the brain involved in mood regulation.
At SNBCare, transcranial magnetic stimulation for depression is offered in an outpatient behavioral health office for adults physically located in Massachusetts or Rhode Island at the time of their appointment. Each patient undergoes a thorough clinical evaluation to determine appropriateness before treatment is considered.
Understanding Transcranial Magnetic Stimulation for Depression
Transcranial magnetic stimulation for depression involves the use of a specialized medical device that delivers focused magnetic pulses to targeted regions of the brain. These regions play a known role in emotional processing and mood regulation.
Because TMS does not involve surgery or systemic medication exposure, many adults explore it as an alternative or complementary option. Additionally, the procedure does not require anesthesia, and patients remain awake and alert throughout each session.
How Transcranial Magnetic Stimulation for Depression Works
TMS for depression works by sending controlled magnetic pulses through the scalp to stimulate neural activity in areas associated with mood regulation. Research suggests that these pulses may help increase activity in regions that appear underactive in individuals with depression.
During treatment:
- A trained clinician positions a magnetic coil near the scalp
- The device delivers brief, repetitive magnetic pulses
- Sessions follow established safety and clinical protocols
As a result, treatment occurs in a structured, monitored outpatient environment.
Who May Be Considered for TMS for Depression
Transcranial magnetic stimulation for depression may be considered for adults who:
- Have a diagnosis of major depressive disorder
- Have experienced limited improvement with antidepressant medications
- Have difficulty tolerating medication side effects
- Are seeking a non-invasive treatment option
- Are currently under the care of a licensed behavioral health provider
However, eligibility is not automatic. Instead, a comprehensive psychiatric evaluation determines whether TMS is clinically appropriate.
Transcranial Magnetic Stimulation and Treatment-Resistant Depression
Some adults experience treatment-resistant depression, meaning symptoms persist despite multiple treatment attempts. In these cases, clinicians may consider transcranial magnetic stimulation as part of a broader care strategy.
At SNBCare, providers do not present TMS as a cure. Rather, they view it as one potential tool within a coordinated mental health treatment plan that may also include therapy and medication management.
What to Expect During Transcranial Magnetic Stimulation for Depression
Initial Evaluation
Before starting transcranial magnetic stimulation for depression, patients complete a detailed psychiatric assessment. This process includes:
- Review of mental health and treatment history
- Discussion of current symptoms and goals
- Evaluation of safety factors and contraindications
- Determination of clinical appropriateness
Only patients who meet established criteria proceed to treatment.
TMS Treatment Sessions
Once treatment begins, patients attend a series of scheduled sessions. Typically, each session lasts under an hour and follows a standardized clinical protocol.
During each session:
- Patients remain awake and seated
- No sedation or anesthesia is required
- The clinician delivers magnetic pulses in controlled sequences
Afterward, most patients resume normal daily activities without downtime.
Safety and Side Effects of Transcranial Magnetic Stimulation
Transcranial magnetic stimulation for depression is generally well tolerated when delivered according to clinical guidelines. Nevertheless, providers review potential risks carefully during the consent process.
Possible side effects may include:
- Temporary scalp discomfort
- Mild headache
- Tingling sensations at the treatment site
Serious side effects are uncommon. Even so, clinicians monitor patients throughout treatment to ensure safety and comfort.
Transcranial Magnetic Stimulation for Depression vs. Medication
Transcranial magnetic stimulation differs from antidepressant medication in several ways. For example:
- It does not involve daily systemic medication use
- It does not rely on gastrointestinal absorption
- It may be considered when medications are ineffective or poorly tolerated
That said, clinicians may recommend TMS alongside medication and therapy rather than as a standalone approach.
Transcranial Magnetic Stimulation and Psychotherapy
Although transcranial magnetic stimulation supports neurological activity, it does not replace psychotherapy. Instead, many adults continue therapy while undergoing TMS.
By combining biological and therapeutic approaches, providers aim to support emotional insight, coping strategies, and long-term mental health stability.
The Role of Behavioral Health Providers in TMS Care
Licensed behavioral health providers guide every stage of transcranial magnetic stimulation for depression. Their responsibilities include:
- Determining clinical eligibility
- Educating patients about treatment expectations
- Monitoring symptom changes over time
- Adjusting care plans when necessary
Importantly, treatment decisions remain collaborative and patient-centered.
Telehealth and Transcranial Magnetic Stimulation for Depression
While TMS sessions require in-person visits, telehealth services may support other aspects of care. For instance, telehealth may be used for:
- Initial psychiatric consultations
- Follow-up appointments
- Medication management
- Therapy sessions
Telehealth services are available only to adults physically located in Massachusetts or Rhode Island at the time of their appointment.
Transcranial Magnetic Stimulation and Sleep Health
Depression and sleep concerns frequently overlap. At SNBCare, behavioral health providers collaborate with an in-house sleep psychiatrist (MD) to support adults whose depressive symptoms involve sleep-related difficulties.
This integrated model allows coordinated assessment and treatment planning within a single outpatient practice.
Why Choose SNBCare for Transcranial Magnetic Stimulation for Depression
SNBCare provides outpatient behavioral health services for adults using evidence-informed, ethical care models. Our approach to transcranial magnetic stimulation for depression emphasizes:
- Comprehensive psychiatric evaluation
- Licensed and experienced clinical providers
- Integrated therapy and medication support
- Clear communication and informed consent
- In-person services in Massachusetts and Rhode Island
All services depend on clinical appropriateness and provider availability.
What Transcranial Magnetic Stimulation for Depression Is Not
To ensure transparency:
- TMS is not guaranteed to work for every individual
- Results vary by patient
- It does not replace emergency mental health care
- It is not offered without proper evaluation
Clear expectations form a critical part of ethical care delivery.
Accessing Transcranial Magnetic Stimulation for Depression at SNBCare
Adults interested in transcranial magnetic stimulation for depression begin by scheduling a psychiatric evaluation at SNBCare. Based on clinical findings and availability, providers discuss appropriate treatment options.
Disclaimer
This content is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. SNBCare provides mental health services exclusively to adults physically located in Massachusetts or Rhode Island at the time of their appointment. All treatments are evidence-informed, supportive, and dependent on provider availability and clinical appropriateness.

